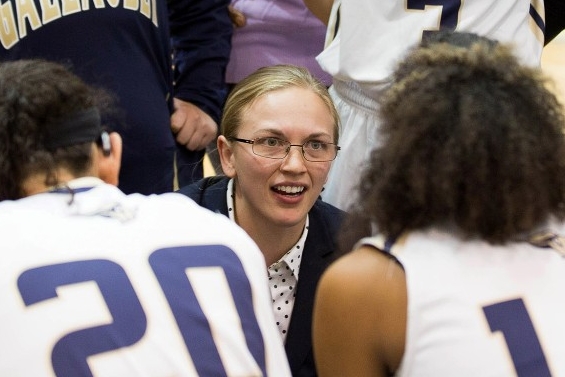Judith Feinberg is drawn to a mess.
Knowing that helps explain why the UC infectious disease doc has boxes of Narcan — the “Lazarus” drug used to revive someone after a deadly overdose of heroin — piled high over her desk on the third floor of Holmes Hospital. Each lifesaving kit will make its way into the hands of a user by way of the mobile needle exchange she started last year.
It took years to get this far, but Feinberg launched the controversial program to stem the spread of hepatitis C and HIV among local drug addicts. While lives have been saved and addicts are even getting clean through the exchange, getting here has been an exhausting battle.
But this fiery physician (pictured at right above) has never backed down from a fight, particularly when it came to looking out for the underserved. Feinberg has spent the last 33 years treating those many others would rather avoid. First it was fighting for the lives of AIDS patients, and now it’s helping heroin addicts. Ironically, the reactions to the epidemics that bookend her career, she says, are frustratingly similar.
“People have all these judgments,” she says, “just like they did about HIV when they said, ‘Oh these people deserve what they get. They did it to themselves.’ People who inject drugs have a parallel story. Addicts are really treated very much the same way (as people with HIV). They are incredibly stigmatized.”
Feinberg completed her infectious disease fellowship at UCLA in the early ’80s where she witnessed firsthand the start of the AIDS epidemic, mostly among young gay men.
“Every time you turned around there would be more and more people in the hospital,” she says. “And they were all young, and they were all dying. And they really were dying horrible deaths. It was hard not to be drawn to it. Everything about it was compelling to me.”
The scientist in her couldn’t pass up the challenge of this new phenomenon, and the humanitarian in her discovered a community of people in desperate need of kindness. “You would see parents deny their sons on their deathbeds,” she recalls.
For decades she chased the disease and eventually became part of the research effort that changed HIV from a death sentence to a manageable chronic condition. Though she is still involved with HIV, today the researcher is fired up for a whole new desperate community — those who find themselves plunging heroin needles, often dirty ones, into their veins.
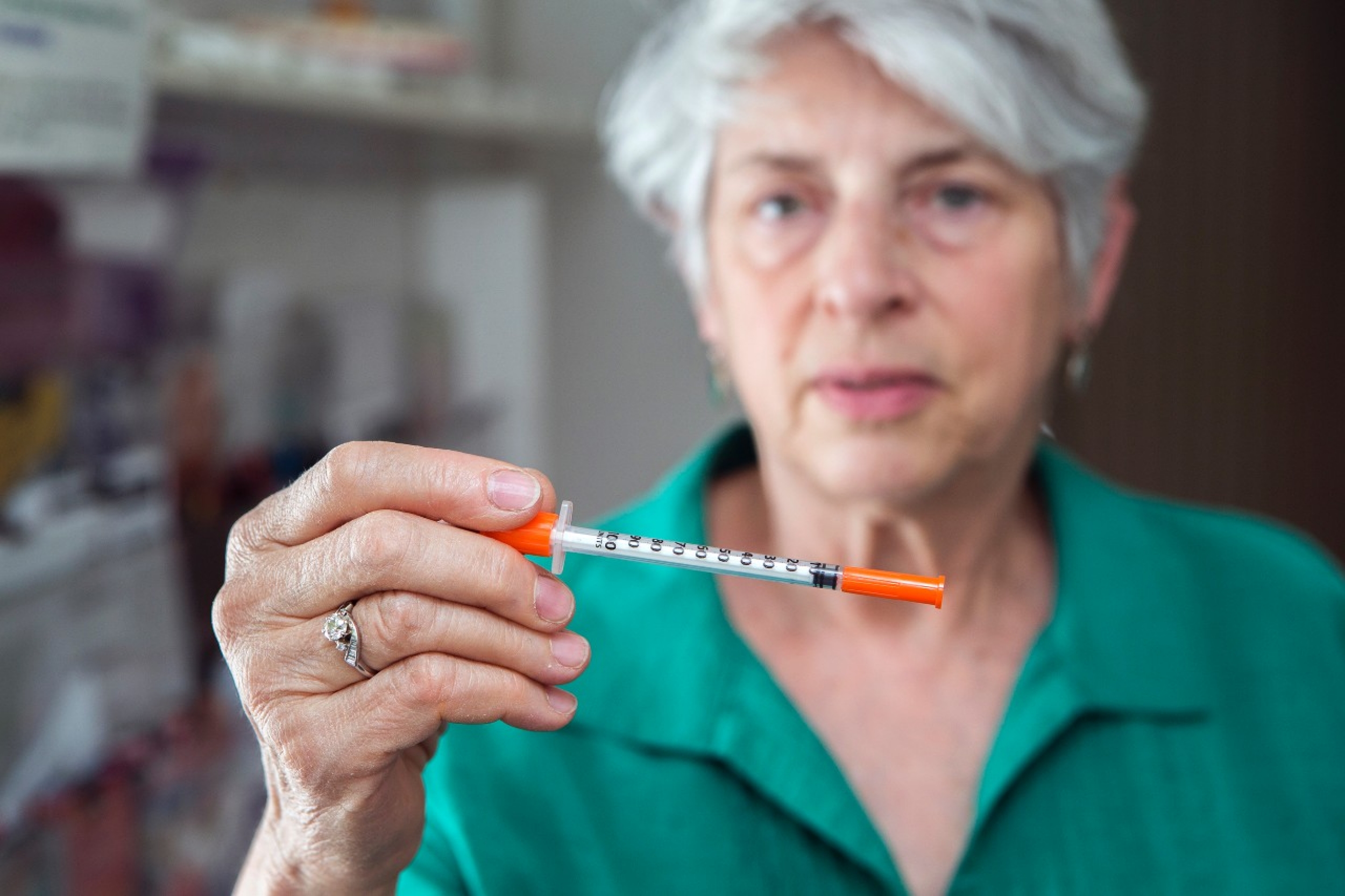
Dr. Judith Feinberg holds up one of the needles that will be distributed to area users. Photos/Andrew Higley
The numbers are startling.
Last year, Hamilton County alone averaged six fatal opiate overdoses a week. That’s more than 300 families a year planning a funeral and burying Cincinnati’s sons and daughters, most of them in their 20s and 30s. Nationally, the drug claims more than 8,000 lives a year.
According to the Centers for Disease Control and Prevention, heroin-related deaths tripled from 2010 to 2013, and the bodies are piling up at the highest rate in Midwestern and Appalachian areas. The Wall Street Journal called it the “scourge of the heartland.”
Feinberg was among the first in Cincinnati to pick up on the area’s heroin issue when a cluster of serious heart infections surfaced among her patients in 2005. The common denominator: injection of opioids. The epidemic, experts say, was fueled when opioid painkillers such as Percocet, OxyContin and Vicodin became harder to obtain — a result of government efforts to curtail prescription drug abuse and to shut down illegal pill mills. Eleven such clinics were shut down in nearby Portsmouth, Ohio, where doctors were doling out pain meds like M&Ms. But the public was already addicted, and dealers — ever the entrepreneurs — moved in with black-tar heroin from Mexico as the next cheap and available fix. A tenth of a gram, usually a dark goo wrapped in a balloon or plastic, brings $10 on the street.
Feinberg approached the dope surge the only way she knew how — as an infectious disease expert. She knew from past experiences at Johns Hopkins in Baltimore that both hepatitis C and HIV would skyrocket if heroin truly took hold in Greater Cincinnati, and she was right. Users in the Tristate were shooting up more and more, but they were also sharing needles and injection paraphernalia, which meant they were spreading disease rapidly. From 2009 to 2013, Hamilton County’s hepatitis C cases increased from 721 to 1,136, a 58 percent increase in four years.
Still, due to political challenges, it took nearly a decade for Feinberg to get a needle exchange approved, funded and on the road. Health departments didn’t want to give the OK, and government officials didn’t want the mobile unit on their streets.
“It should not have taken nine damn years to tell people, ‘Look, we’ve got a public health problem here,’” the former New Yorker says in her direct style. “I can’t tell you what all people said to me, but people in public office that we had elected would say, ‘They are junkies. If they die — fewer junkies.’ I mean that’s what people said about gay men, too. ‘If they die — fewer gay men, the world will be a better place.’
“But here is the problem, the oath I took when I graduated medical school was not the ‘just-let-’em-die oath.’ When you see a patient with lung cancer from smoking, you don’t go in there and say, ‘You deserved this.’ It is not our job to judge. It is our job to take care of sick people.”
Feinberg finally started the Cincinnati Exchange Project (CEP) on a shoestring with a $50,000 grant from Interact for Health, a local foundation, in February 2014. But even after it got going, the first community to invite them in — Springdale, Ohio — pulled the plug after six weeks when area groups and residents protested.
Through August of this year, the CEP had met with about 450 clients in the few Cincinnati neighborhoods — Northside, Walnut Hills and Mount Auburn — that allow the exchange to park its donated 1997 motor home and open up for a few hours each week. In 18 months, they exchanged 45,000 needles.
The project received an additional $48,000 two-year grant in 2014 from the Ohio Department of Health that enables them to provide nasal naloxone (trademarked as Narcan) to drug users and their families to prevent fatal overdoses. Once administered, the drug counters life-threatening depression of the central nervous system and allows the victim to breathe normally again. At last count, 68 of the kits had been used, and they only know about those because clients came back for more.
“For $74,000, we have saved 68 lives,” says Feinberg. “I mean, it is quite a bargain. These people deserve a chance. You can’t go into rehab if you aren’t breathing. You can’t be rehabbed if you are dead.”
Libby Harrison, a former heroin user herself, serves as the program manager for the exchange and oversees the on-site operation in the RV, which heads into the community for three hours every Monday, Wednesday and Thursday.
Clients come in all forms, Harrison says, but nearly all are white, and more than half have jobs. On average, they spend around $50 a day on their habit.
“A lot of them drive in from the suburbs,” says Harrison. “People get this idea of what a drug addict is from Hollywood.” Just as there are functional alcoholics, she says, there are plenty of functional drug addicts.
Besides providing clean equipment, Harrison, who posts her cellphone number on the exchange’s website, also shares vein care advice and drug treatment options. Of the more than 450 heroin addicts they have helped, around 10 percent — or roughly 45 people — have sought treatment and gotten clean.
The exchange also provides on-the-spot testing for hepatitis C and HIV, which revealed that more than seven in 10 of their clients test positive for hepatitis C while 4 percent test positive for HIV. Feinberg estimates the cost of curing a single person of hepatitis C averages $125,000. Costs escalate exponentially if left untreated as patients, often decades later, develop cirrhosis then liver cancer and eventually require a liver transplant to survive.
"...the oath I took when I graduated medical school was not the ‘just-let-’em-die oath.’ It is not our job to judge. It is our job to take care of sick people.
‒ Dr. Judith Feinberg
The key to reducing the spread of these diseases among injection drug users, experts maintain, is to educate users and equip them with clean needles. In addition, the exchange provides users with “cookers” and bits of cotton used to heat and filter the drug because hepatitis C lives on inanimate surfaces for days to weeks. The state of Indiana reversed its ban of syringe exchanges this year after a spike of 170 new cases of HIV among drug users in one southern county within a six-month period. And Northern Kentucky is pursuing an exchange after hospitals there reported more than 700 heroin overdoses in 2014.
While some maintain that handing out clean needles and paraphernalia encourages drug use, Feinberg scoffs, and points to dozens of studies that show syringe exchanges decrease drug use and get people into drug treatment.
“That is like saying that the existence of a mug facilitates alcoholism,” she says as she holds up the coffee cup from her desk. “If people want to drink straight from the bottle, they can. If an addict wants to shoot up, they will shoot up whether they have a clean needle or not. They will find needles in the street or whatever it takes.”
Harrison knows a thing or two about doing whatever it takes. She has even accompanied 20 or more of their clients to treatment. In those instances, the addict is normally “dope sick” and in withdrawal because treatment centers typically require them to be clean at least 24 hours before arriving.
“It is like the worst flu you have ever had, then multiply that by 10,” says Harrison. “It is a really rough place to be. It is awful, and your brain is misfiring because it is missing certain chemicals, and it is only telling you to go get drugs.
“I want them to have somebody who is taking care of them and shows up and holds their hand and makes sure they actually get there. They are sweating and throwing up. They can’t think and are generally crying, even the big burly men, because their emotions are so screwed up.”
Harrison sees the exchange as an opportunity to help people own their health care, but she also knows of seven former clients — those she cared for and cared about — who have died of an overdose. “We have lost some,” she pauses.
“Most of them are amazing wonderful people, and they deserve a chance. Heroin addicts are usually treated horribly. We get to be the place where they are loved, and having someplace where they can come and be loved knocks down some of the shame barrier.
“They are not going to go to treatment if they hate themselves. Nobody wants to be an addict.”
LINK:
Learn more about the Cincinnati Exchange Project

John Bach
As editor of UC Magazine, John enjoys the opportunity to put a human face on a large institution by telling compelling stories of the University of Cincinnati's incredible community of alumni, faculty, staff and students.
John.Bach@uc.edu
Additional Credits: Special thanks to photographer Andrew Higley, web developers Ben Stockwell and Kerry Overstake as well as designers Ben Gardner and Kathy Bohlen for helping to develop and present the rich multimedia content contained in this piece. Heroin deaths chart data taken from the Centers for Disease Control report.
More from this issue:
The haze after the blaze
Veteran's personal experiences help him relate to students struggling with reintigration.